Are Consecutive Decreasing Blood Pressure Readings Valid
Abstract
We evaluated the consequences of excluding the first of three blood pressure (BP) readings in different settings: a random population sample (POS, n=1525), a general practice office (GPO, n=942) and a specialized hypertension middle (SHC, due north=462). Differences between systolic and diastolic BP (SBP and DBP) estimates obtained including and excluding the outset reading were compared and their correlation with convalescent BP monitoring (ABPM) was estimated. The samples were divided into quartiles co-ordinate to the difference betwixt the 3rd and the get-go SBP (3-1ΔSBP). SBP decreased through sequential readings, 3-1ΔSBP was −5.v±9.7 mm Hg (P<0.001), −5.1±x.iv mm Hg (P<0.001) and −half dozen.one±9.3 mm Hg (P<0.001) for POS, GPO and SHC, respectively. Still, individuals included in the meridian quartile of three-1ΔSBP showed their highest values on the tertiary reading. The hateful SBP estimate was significantly higher excluding the commencement reading (P<0.001), but the differences amid both approaches were small (i.v–1.half dozen mm Hg). Moreover, the correlation betwixt SBP values including and excluding the first reading and daytime ABPM were comparable (r=0.69 and 0.68, respectively). Similar results were observed for DBP. In conclusion, our study does not support the notion of discarding the first BP measurement and suggests that it should be measured repeatedly, regardless the offset value.
Introduction
Accurate function blood pressure (BP) measurement remains the mainstay of the diagnosis and handling of hypertension, and the BP estimate in the first visit is the cornerstone of the initial management of hypertension as these values will be used to decide if subsequent visits are necessary. The recognition of a reduction in the white-coat effect through successive measurements of BPone has led to the suggestion that discarding the first function reading of a set of three may improve the possibility of knowing the actual BP. If BP ever decreases in the subsequent measurements, boosted BP readings are not necessary when the beginning measurement is <140/90 mm Hg. Even so, the assumption that the kickoff BP reading is systematically college in all subjects was non widely studied. Two guidelines aimed at improving hypertension diagnosis and treatment in the clinical practice were recently published, the '2013 European Order of Hypertension (ESH) and of the European Society of Cardiology (ESC) guidelines for the management of arterial hypertension'two and the '2013 Canadian Hypertension Education Program (CHEP) Recommendations for Claret Pressure Measurement, Diagnosis, Assessment of Hazard, Prevention, and Treatment of Hypertension'.three They concur on a value of ⩾140/90 mm Hg equally hypertension threshold, just at that place is disagreement regarding whether the commencement reading should be discarded or non. The ESH/ESC guidelines recommend taking 'at least two BP measurements, in the sitting position, spaced i–2 min apart, and additional measurements if the first ii are quite different'. On the other hand, the Canadian guidelines suggested that 'At the initial visit for the assessment of hypertension, if systolic BP is ⩾140 and/or diastolic BP is ⩾90 mm Hg, more than than 2 additional readings should be taken during the same visit' and 'The first reading should be discarded and the latter 2 readings averaged'.
Disagreement about whether to discard the first BP measurement or not was also observed in population studies; for example, two recently published studies aimed at evaluating the variability of BP in the general population—both based on National Wellness and Diet Examination Survey (NHANES) information—estimated the BP using different criteria: the kickoff used the average of the second and third measurement4 whereas the other used the average of the 3 readings.five
The aim of our study was to evaluate the effect of discarding the starting time BP measurement. For this purpose the BP estimates including and excluding the first reading were compared in three dissimilar settings: (a) a random population sample, (b) a screening for loftier BP in general practice offices (GPOs) and (c) a specialized evaluation in a hypertension center. In the terminal setting we also evaluated whether discarding the get-go BP reading improves the human relationship betwixt role BP and ambulatory BP monitoring (ABPM) equally was previously suggested.
Materials and methods
The written report was performed using data from individuals who had had at least three consecutive BP readings on one occasion from 3 independent samples, (1) a random population sample, (2) sequent patients in a GPO and (3) consecutive patients in a specialized hypertension center (SHC).
The methodology used in the random population sample to obtain measurements has already been published.6,7 In cursory, 3 BP measurements spaced effectually two min from one another were performed at dwelling house by trained nurses, after a minimum resting period of 5 min, using a mercury sphygmomanometer. Phase I and 5 Korotkoff sounds were used to identify systolic BP (SBP) and diastolic BP (DBP) respectively.
In the GPOs, doctors using the OMRON HEM 705 CP devices (OMRON HEALTHCARE Co., Kyoto, Japan) took three BP measurements separated by a minute in a unmarried visit from every patient examined regardless of the purpose of the visit.
In the SHC particularly trained nurses performed three BP measurements just before the realization of ABPM with the same device and methodology used in the GPO setting. The ABPM registries were performed with the SpaceLabs 90207 monitor (Spacelabs Healthcare, Issaquah, WA, U.s.a.) programmed to read BP at intervals of 20 min during the day and 30 min during the night. Day and night was differentiated past taking into account the patient'due south diary.
To analyze the BP behavior through successive readings and evaluate if the first reading was systematically highest, mean and quartiles of the deviation between the third and commencement SBP (iii-1ΔSBP) and DBP (iii-1ΔDBP) readings were estimated. In order to determine the effects of antihypertensive drugs, individuals with and without treatment were analyzed separately. Age and body mass index were compared among quartiles of three-1ΔSBP using analysis of variance with Tukey post hoc analysis, and sex activity and electric current smoking using χ 2-test.
To judge the effect of discarding the first BP reading, mean BP was estimated in each subject using two different approaches: (1) discarding the start measurement and (2) averaging the 3 readings.
Differences between SBP and DBP values obtained using both approaches were calculated and compared using one-sample t-test. Too, for each sample, Bland–Altman plots were constructed with the difference of the two approaches on the vertical axis and the boilerplate of the 2 approaches on the horizontal axis. Horizontal reference lines on the scatterplot showed the difference between the measurements ±2s.d. In social club to investigate the concordance of high BP diagnosis (SBP⩾140 mm Hg and/or DBP⩾ninety mm Hg) among both BP estimates, we calculated the kappa coefficient (κ) after dichotomizing the role measurements every bit 'high' or 'depression' BP. The prevalence of high BP both including and excluding the starting time BP reading were compared using McNemar'south test.
Finally, in the SHC sample, the relationship between the office BP values obtained and the mean daytime ABPM were evaluated using Pearson correlation coefficient (r); additionally, 95% conviction intervals (95%CI) for r values were calculated based on the Fisher r-to-z transformation.
Statistical analyses were performed using SPSS eighteen.0 software (SPSS, Chicago, IL, USA); ii-tailed P-values <0.05 were considered statistically significant.
Results
The study included 2926 individuals (1780 women, 46±17 years old and 1149 men, 47±17 years former, P betwixt sex=0.566). The characteristics of the three samples are described in Tabular array 1.
As Tables 2 and 3 prove, mean BP decreased beyond the sequential readings; the mean decrease was like in all settings; Δ3-1SBP was −5.5±9.7 mm Hg (P<0.001), −5.1±10.4 mm Hg (P<0.001) and −half dozen.i±ix.iii mm Hg (P<0.001) in the random population sample, GPO and SHC, respectively; Δ3-1DBP was −3.0±ix.0 mm Hg (P<0.001), −1.71±7.8 mm Hg (P<0.001), and −ii.one±5.7 mm Hg (P<0.001) in the random population sample, GPO and SHC, respectively. However, when the samples were divided into quartiles of the Δ3-1SBP, the individuals included in the tiptop quartile had college SBP values in the tertiary reading compared with the first one (Figure 1a); similar behavior was observed with DBP when it was divided into quartiles of Δ3-1DBP (Figure 1b). Individuals in the height quartile of Δ3-1SBP were younger (46±xviii vs 49±16 years old, P=0.007) and thinner than individuals in the first quartile of (trunk mass index 26.7±5.4 vs 28.1±6.half-dozen, P<0.001). The per centum of current smokers was higher in the meridian quartile of Δ3-1DBP than in the remaining quartiles (26.4 vs 22.six, P=0.034). The pct of women was similar amidst quartiles of Δ3-1SBP (61.2, 62.5, 61.6 and 58.0, P=0.284).
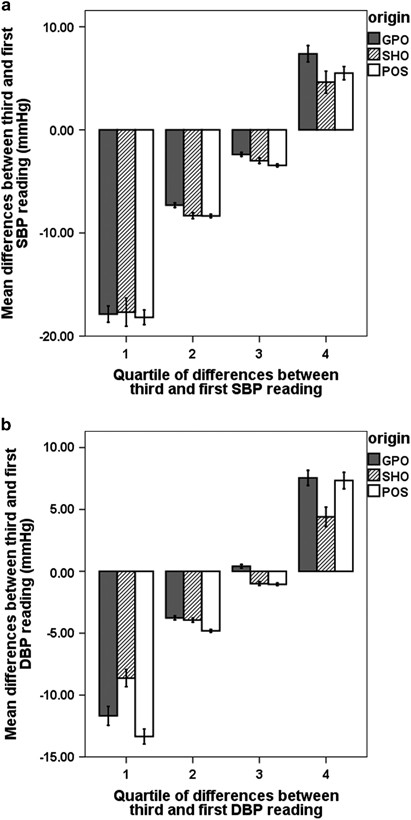
Mean differences between the tertiary and the first SBP (a) and DBP (b) readings according to quartiles of these differences in the three samples analyzed: random population sample (POS), full general practice office (GPO) and specialized hypertension office (SHO).
Tables 2 and iii also compare the difference between the hateful of all readings and the mean excluding the first reading; SBP and DBP were significantly lower in all settings when the first reading was discarded. Although the mean differences for SBP including and excluding the showtime BP reading seem merely modest, 1.v (iii.0), 1.6 (2.eight) and 1.6 (two.eight) mm Hg for GPO, specialized hypertension and office random population sample, respectively (Table ii), the range was wide, and included positive and negative values (from −thirteen.three to 27.three mm Hg) (Figure 2, Bland–Altman plots). Therefore, excluding the kickoff reading did not yield lower values systematically. Similar results were obtained for DBP (Tabular array three); the mean differences between BP estimates were 0.5 (2.iii), 0.six (i.7) and 0.eight (2.half-dozen) mm Hg for GPO, specialized hypertension and part random population sample, respectively.
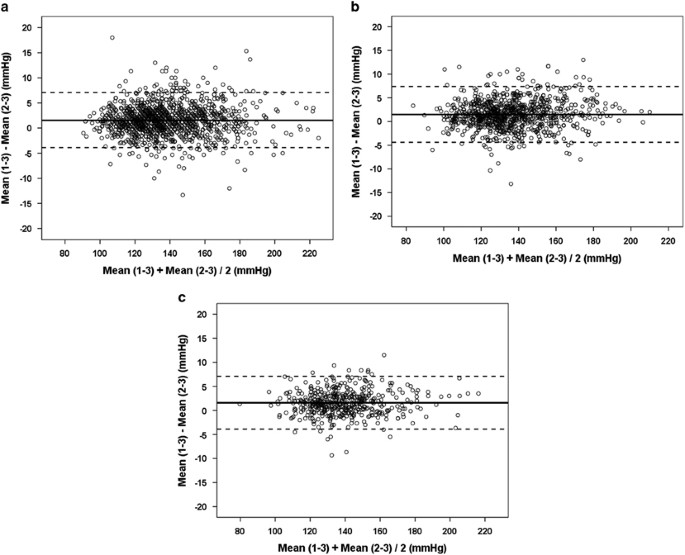
Banal–Altman plots comparing the SBP approximate using the mean of three readings and discarding the get-go reading in the 3 samples analyzed: random population sample (POS) (a), general practice function (GPO) (b) and specialized hypertension function (SHO) (c).
The proportion of individuals with 'high' BP (⩾140/90 mm Hg) was lower when the first reading was excluded in all settings (42.3% vs 44.6% in the random population sample, P<0.001, 42.three% vs 44.3% in the GPO, P=0.005 and 45.five% vs 48.seven% in the SHC, P=0.001). However, the concordance between approaches was loftier (κ=0.90, 0.91 and 0.91 for the random population sample, the GPO and the SHC, respectively); indeed, 2794 of 2929 subjects were classified concordantly; among the 135 subjects classified discordantly, 75.6% were considered as 'high' BP only when the mean of all 3 readings was used and 24.4% when the first BP reading was excluded.
In the SHC sample, 446 ABPMs were considered valid. The correlations between daytime systolic ABPM and both approaches to judge office SBP were modest merely similar, r=0.69 (95% CI 0.64–0.73, P<0.001) and r=0.68 (95% CI 0.61–0.73, P<0.001), for the mean of three readings and excluding the first measurement, respectively (Effigy 3). The correlations between daytime diastolic ABPM and office DBP estimates were also similar, r=0.69 (95% CI 0.64–0.73, P<0.001) and r=0.68 (95% CI 0.63–0.73, P<0.001), respectively.
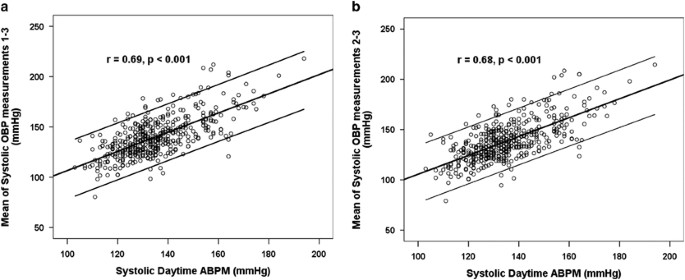
Pearson'due south correlation betwixt systolic daytime ambulatory blood pressure monitoring (ABPM) and the office systolic claret pressure level (OBP) estimate obtained using (a) the mean of three readings and (b) discarding the first reading.
Discussion
Accurate office BP measurement, despite its shortcomings, remains the mainstay of diagnosis and treatment of hypertension. All the same, the elementary question of whether the kickoff part BP measurement should exist discarded remains to be answered and there is no agreement among the varying hypertension guidelines. Thus, the Canadianthree and Prissy8 guidelines recommend discarding the starting time BP measurement, whereas the ESH/ESC i does non.two Our data bear witness that, in all settings analyzed, the event of excluding the showtime BP reading was meaning but modest, ~1.5 and <1 mm Hg for SBP and DBP, respectively. Moreover, when BP was analyzed as a dichotomic variable in society to classify subjects as 'loftier' or 'low' BP, the vast bulk were classified concordantly.
Information technology has been suggested that excluding the start BP measurement could improve the correlation between office BP and out of the office BP. All the same, our data do not back up this concept; using the second and 3rd readings but (that is, discarding the beginning) did not amend the correlation with daytime ABPM when compared with the use of mean of all three readings; indeed, r values were almost identical whether the outset BP measurement was included or not. This statement is concordant with a previously published study about untreated hypertensive patientsnine but expands the determination to not-hypertensive subjects and to subjects using antihypertensive drugs.
The subtract of BP in successive measurements has been shown repeatedly and with different methods,10 and it is widely internalized in medical thinking that successive measurements will give lower BP values. Thus, Parati et al. iv suggested that discarding the kickoff reading may amend the accuracy of the diagnosis of hypertension. Furthermore, in gild to eliminate the increase of BP associated with the effect of alarm, ESH guidelines for home BP measurement recommend discarding the measurements performed on the first twenty-four hours.11 Nevertheless, the scientific show to back up these assumptions is minimal and valuable information nearly BP variability could be lost.
Perhaps the well-nigh interesting finding in our study was the fact that ~25% of the individuals did not decrease or increase their BP trough successive measurements and, consequently, in these individuals the first reading was not the highest. Remarkably, this beliefs was found in all three settings (population sample, general practice and specialized hypertension office) and it was as well independent of whether BP was measured by medical doctors or nurses, in the office or at home. Despite this phenomenon beingness previously published,12 it is non widely recognized and it has several implications for clinical practice.
First, the consequences of excluding the initial reading are unpredictable for an individual patient. As Bland–Altman plots testify, the differences among BP approximate excluding or including the beginning measurement were wide, and yield both positive and negative values. Indeed, although the individuals who increased their BP in the third reading were younger, thinner and more current smokers than those who decreased BP trough successive measurements (first quartile of three-1ΔSBP), in that location are no practical means to place them. Interestingly, the reclassification of individuals in categories of BP using the mean of the kickoff and second, first through 3rd, and 2nd and third readings was recently published.13
Another related effect is whether or not a medico should take more than readings only when the offset is ⩾140/ninety mm Hg as the NICE guidelines and Canadian recommendations suggest; our findings practise non support this approach. As the cardiovascular risk has a continuous relationship with BP starting with values as depression every bit 115/75 mm Hg,14 taking only one BP measurement could significantly underestimate the field of study'south 'true' risk of cardiovascular event.
Finally, the difference between the kickoff and tertiary reading could requite some of import information about the BP variability. There is now some evidence that several such representations of BP variability, if augmented, increment cardiovascular risk independent of the average of BP readings conventionally acquired.xv Visit-to-visit SBP variation was linked to increased cardiovascular and stroke mortality risk.16 Although the chance associated with the short-term variability has been studied less, the BP variation in 1 visit results from changes in eye rate, stroke volume and peripheral resistance in response to external and internal stimuli and their importance in terms of the take chances of developing hypertension or cardiovascular disease remain to be defined.
Some limitations of our written report have to be pointed out. First, this was a mail service hoc analysis. 2nd, this written report was performed in different settings with different methodologies to measure BP. However, our findings were concordant through all the samples, suggesting that the BP patterns observed were strongly consistent. Finally, our study was not able to define whether one approach would be more than advisable than some other; only long-term prospective studies with hard end points could provide a definitive answer.
In conclusion, our study does not support discarding the first BP measurement equally the Canadian and NICE guidelines take suggested. Remarkably, although the mean BP decreased in successive BP readings, the beliefs of individuals was unpredictable and an appreciable proportion of subjects had the highest BP value in the last reading. Nosotros suggest that 3 BP readings should be taken in all individuals independently of the first reading value.

References
-
Parati G, Mancia G . Assessing the white coat effect: which blood force per unit area measurement should be considered? J Hypertens 2006; 24: 29–31.
-
Mancia 1000, Fagard R, Narkiewicz Thousand, Redón J, Zanchetti A, Böhm M et al. 2013 ESH/ESC Guidelines for the management of arterial hypertension: the task strength for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Club of Cardiology (ESC). J Hypertens 2013; 31: 1281–1357.
-
Hackam DG, Quinn RR, Ravani P, Rabi DM, Dasgupta K, Daskalopoulou SS et al. The 2013 Canadian Hypertension Teaching Programme recommendations for blood pressure measurement, diagnosis, cess of risk, prevention and handling of hypertension. Tin can J Cardiol 2013; 29: 528–542.
-
Muntner P, Shimbo D, Tonelli M, Reynolds K, Arnett DK, Oparil S . The human relationship between visit-to-visit variability in systolic blood pressure and all-cause mortality in the general population: findings from NHANES Iii, 1988–1994. Hypertension 2011; 57: 160–166.
-
Muntner P, Levitan EB, Reynolds K, Mann DM, Tonelli Grand, Oparil S et al. Within-visit variability of blood pressure and all-cause and cardiovascular mortality among U.s. adults. J Clin Hypertens (Greenwich) 2012; 14: 165–171.
-
Salazar MR, Carbajal HA, Aizpurúa G, Riondet B, Rodrigo HF, Rechifort V et al. Decrease of blood pressure by community-based strategies. Medicina (B Aires) 2005; 65: 507–512.
-
Salazar MR, Carbajal HA, Espeche WG, Aizpurúa M, Leiva Sisnieguez CE, March CE et al. Identifying cardiovascular illness risk and outcome: utilize of the plasma triglyceride/high-density lipoprotein cholesterol concentration ratio versus metabolic syndrome criteria. J Intern Med 2013; 273: 595–601.
-
National Clinical Guideline Centre (United kingdom of great britain and northern ireland). Hypertension: The Clinical Management of Main Hypertension in Adults: Update of Clinical Guidelines eighteen and 34 [Cyberspace]. Regal College of Physicians (UK): London, 2011.
-
Graves JW, Grossardt BR . Discarding the first of 3 nurse-auscultatory or oscillometric claret force per unit area measurements does not improve the association of office blood pressure with ABPM. Claret Printing Monit 2010; 15: 146–151.
-
Mengden T, Hernandez Medina RM, Beltran B, Alvarez E, Kraft M, Vetter H . Reliability of reporting self-measured blood pressure values by hypertensive patients. Am J Hypertens 1998; 11: 1413–1417.
-
Parati Thou, Stergiou GS, Asmar R, Bilo Grand, de Leeuw P, Imai Y et al. ESH Working Group on Blood Pressure Monitoring European Society of Hypertension exercise guidelines for abode blood force per unit area monitoring. J Hum Hypertens 2010; 24: 779–785.
-
Graves JW, Grossardt BR, Gullerud RE, Bailey KR, Feldstein J . The trained observer meliorate predicts daytime ABPM diastolic blood pressure in hypertensive patients than does automatic (Omron) device. Blood Press Monit 2006; xi: 53–58.
-
Handler J, Zhao Y, Egan BM . Impact of the number of blood pressure measurements on blood force per unit area classification in US adults: NHANES 1999–2008. J Clin Hypertens (Greenwich) 2012; 14: 751–759.
-
Lewington S, Clarke R, Qizilbash North, Peto R, Collins R . Prospective Studies Collaboration. Age-specific relevance of usual claret pressure to vascular mortality: a meta-analysis of individual information for one million adults in 61 prospective studies. Lancet 2002; 360: 1903–1913.
-
Floras JS . Blood pressure variability: a novel and of import risk factor. Tin can J Cardiol 2013; 29: 557–563.
-
Kikuya M, Ohkubo T, Metoki H, Asayama One thousand, Hara A, Obara T et al. Day-by-day variability of blood pressure and heart rate at home as a novel predictor of prognosis: the Ohasama Study. Hypertension 2008; 52: 1045–1050.
Acknowledgements
This study could not have been conducted without the aid of the nurses from the 'Hospital Municipal, San Andrés de Giles' and the 'Hospital Municipal, Rauch' and the nurse Miriam Susana Cor from the 'Hospital Universitario San Martín, La Plata'. Nosotros appreciate the help of Sonja Zander in the revision of the English language of this manuscript.
Author data
Affiliations
Corresponding author
Ideals declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this commodity
Salazar, Grand., Espeche, W., Aizpurúa, Yard. et al. Should the first blood force per unit area reading be discarded?. J Hum Hypertens 29, 373–378 (2015). https://doi.org/10.1038/jhh.2014.98
-
Received:
-
Revised:
-
Accepted:
-
Published:
-
Issue Appointment:
-
DOI : https://doi.org/10.1038/jhh.2014.98
Source: https://www.nature.com/articles/jhh201498
0 Response to "Are Consecutive Decreasing Blood Pressure Readings Valid"
Post a Comment